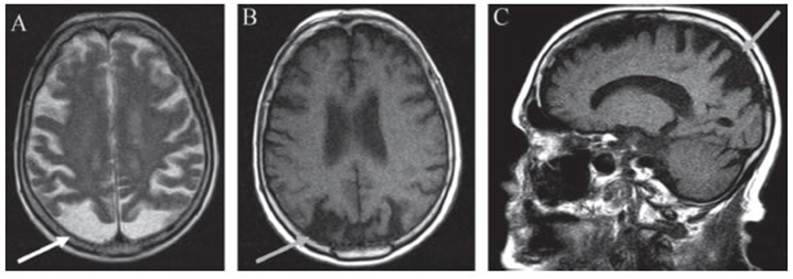
We report the case of an 89-year-old woman who has had confusion and agitation for three years. She was un der follow-up with a diagnosis of Alzheimer’s disease, receiving quetiapine 25 mg/day, with worsening of symp toms in agitated environments. She reported visual prob lems for 20 years and has been getting worse ever since. The patient underwent magnetic resonance imaging that revealed atrophy of the bilateral cortical superior parietal lobe “in a mirror” (Fig. 1, arrows), suggesting Benson’s Syndrome, and signs of leukoaraiosis/microangiopathic leukoencephalopathy and encephalic volumetric reduc tion. Posterior cortical atrophy or Benson’s syndrome is a neurodegenerative dementia marked by a progressive interruption of visual abilities in addition to atrophy of the parietal and occipital regions. Both prevalence and heredity are still unknown as it is a rare subtype of Alzheimer’s disease (5% of cases). The diagnosis is proposed by some criteria, such as insidious onset with visual or visuospatial dysfunction in the absence of justifiable ophthalmopathy; complex visual disorder with difficulty reading, optic ataxia, ocular apraxia, simultanagnosia, vi sual agnosia, spatial disorientation; progressive charac ter changes; less involvement of memory and language; imaging demonstrating unilateral or bilateral occipital-parietal or occipital-temporal atrophy, hypometabolism or hypoperfusion.