INTRODUCCIÓN
The Birt-Hogg-Dubé (BHD) syndrome is a rare clinical-pathological entity of autosomal dominant inheritance, described in 1977 by Birt et al, cha racterized by skin neoplasia, generally skin-colored soft papules on the face, neck and ears, with lung cysts and renal neoplasia.1,2
Up to now, more than 140 mutations in the gene related to this clinical entity have been described. The gene is known as “FLCN”, and is located in the chromosome 17p11.2, which encodes folliculin, a pro tein expressed in multiple tissues including the skin, type I pneumocytes, and the distal nephron, whose exact function is unknown, but seems to act as tumor suppressor by interacting with the pathway of the mTOR (mechanistic target of rapamycin) protein, the tissue growth factor beta and the DENN (diffe rentially expressed in normal and neoplastic cells) protein.1-3 In this article we report two cases of BHD.
Case number 1
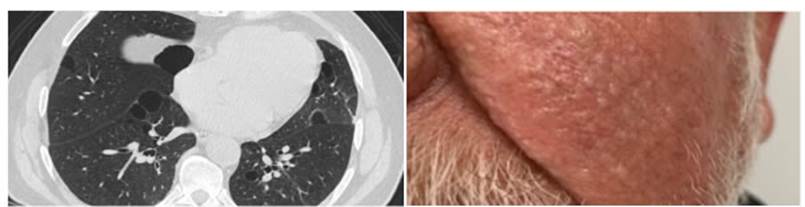
Female patient, 68 years old, with history of hys terectomy due to cervical cancer 20 years ago. Thirteen years later, she required a nephrectomy due to clear cell renal carcinoma; subsequently, after two years, she showed yellowish pigmented papules on the face, thorax and forearms, thus, she was assessed by dermatologic testing one year later (Figure 1). The patient underwent biopsies of the papules on the left nasal ala and anterior trunk, with histopathological findings compatible with angiofibromas, and then received urology and dermatologic testing without new findings or symptoms. Given the presence of multiple tumors, she was evaluated through genetic testing and underwent an axial chest high-resolution com puted tomography (HRCT) that identified some lung nodules of less than 1 cm and multiple, well-defined bilateral lung cysts of variable size, with lens (lenticular) or round shape, some subpleural and others, septated. So, a FLCN gene mutation study was carried out, and found a mutation of the exon 11/18, variant c. 1285del, pathogenic, thus confirming the diagnosis of the Birt-Hogg-Dubé syndrome (Figure 1). The patient was referred to the Pulmonology Department for a complementary evaluation. She was in good general condition, without respiratory difficulties or any other asso ciated symptom.
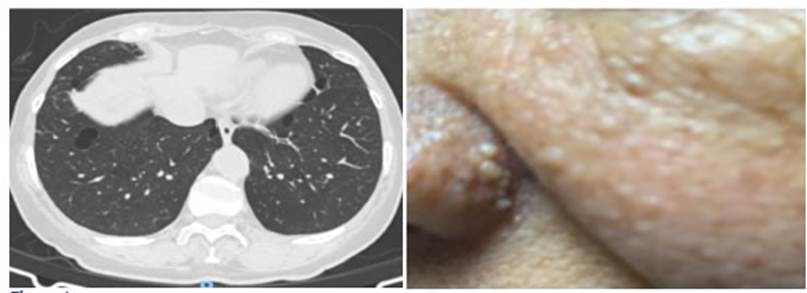
Figure 1 Case 1: chest HRCT showing well-defined bilateral lung cysts of variable size, of round or lenticular shape, some sub pleural and others, septated, known as “alveolus in the alveolus”, and image of the patient showing lesions suggestive of fibrofol liculoma in the nasal ala and maxillary region.
Case number 2
Male patient, 72 years old, light smoker with a pack year index of 5 during 10 years, history of prostate cancer, treated with radiation therapy and prostatectomy 9 years ago. Three years later, the patient showed cough and dyspnea with great effort, of one month of evolution, and was referred to the Pulmonology Department. The physical exam showed multiple smooth surface papule lesions on the face, pedunculated brownish hy perpigmented smooth surface papules on the neck and external side of the right eye, and well-defined pigmented plaque, greasy to the touch, on the chest (Figure 2). The rest of the physical exam was normal, including lung auscultation. A spirometry was performed with normal results, also a HRCT that showed two bullae and multiple lung cysts of different sizes, some rounded and others with the form of a lens (lenticular), which increased in number towards the bases, with the “alveolus in the alveolus” pattern (cysts with internal septa) (Figure 2). Due to all those findings, the patient was referred to the Dermatology Department for a biopsy of the skin lesions. Biopsies taken from the lesions on the forehead, the ear, and left cheek are compatible with tricofolliculoma. Two years later, a renal ecography was performed, which showed a complex renal cyst in the lower pole of the left kidney and multiple bilateral simple cysts, and a tomographic study showed similar findings. A new ecographic control carried out 2 years later identified a stable lesion when compared to the previous study. In that case, the BHD diagnosis was confirmed, in accordance with clinical and histopathological findings of the skin biopsy. At present, the Pulmonology Service performs the clinical follow-up; the patient doesn’t show acute symptoms and has occasional coughing.
DISCUSSION
The BHD is a rare autosomal dominant disorder caused by a mutation in chromosome 17 of the fo lliculin gene; however, the physiopathological me chanism involved is yet unknown.4 Some studies suggest that it causes hyperactivity of the mTor pathway and increases the production of growth factors and aminoacids, which is considered the cause of carcinomas and lung cysts.5
The most common genetic mutations belong to c.1285dup/ c.1285dup + c.1285del (as the one identified in case 1), c.1300G > C and c.250- 2A > G. Mutations in c.1285delC or c.1285dupC account for 50% of BHD cases, whereas the other muta tions are associated with an increase in the risk of pneumothorax, present in up to 77% of the cases.4,6
Skin lesions appear between the third and fourth decade of life, and present with the classic triade of fibrofolliculoma, tricodiscomas and acrochordons in 90% of the cases. The lesions measure from 1 to 5 mm, and generally appear on the nose, the nasolabial folds, the cheeks, the forehead, the upper trunk, the ear lobe and the retroauricular area.1,7
80% of patients show lung cysts.2 The HRCT shows well-defined, thin-walled cysts, usually multiple and bilateral, predominantly basal (lower lobes), paramediastinal or subpleural, of variable size, but the most predominant measure 1 cm. They can be rounded or lentiform, but the mor phology changes according to size: the bigger the cyst, the lower the probability of it being rounded, and the higher the probability of it having the “alveolus in the alveolus” pattern. These are cysts with internal septa.8
The real cause of the cysts is unknown. The hypothesis about the stretching has been posed, suggesting there are adhesion defects and that due to repeated hyperinflation, the alveolar space expands2,4 There isn’t gender predilection, they tend to appear from the third decade of life. They can be complicated by pneumothorax in 20%-30% of the cases, though it varies in familial cohorts, considered to have fifty times higher risk of pneu mothorax than the general population, but it is much lower compared to other entities such as lymphangioleiomyomatosis, where the risk is a thousand times higher.1-4,7,9,10
In patients with BHD, the incidence of renal cancer increases seven times more than in persons not affected by this syndrome, and generally tu mors appear in the fifth decade of life. Variations have been described regarding the appearance of the tumors, from 6.5% to 34%; they may be unilateral or bilateral, and the syndrome tends to be more common in males. The most common are hybrid oncocytic tumors and chromophobe carcinoma (50%-80%).1,2,4 Simple renal cysts have also been reported, but since these are common in the general population, no clear association has been shown.4
The diagnosis is usually delayed, even for years, missed or wrong, since it can be confused with other causes of spontaneous pneumothorax; and it is challenging, given the high genetic and clinical variability: up to 25% of asymptomatic carriers, older than 20 years, without skin lesions, or sub groups that show some mild fibrofolliculomas.12 The main differential diagnosis is lymphangio leiomyomatosis associated with tuberous sclerosis, due to similarities regarding the lung cysts, and skin and renal tumors.4,13
Patients with suspected BHD must be evaluated with a HRCT for the analysis of lung cysts and pneumothorax, and with abdominal CT or renal ecography at the time of the diagnosis; also tomo graphic follow-up must be carried out at least every three to five years. We recommend the screening of first-degree relatives of affected individuals aged 20 and upwards; and starting from 40 years, routine screening for renal disease shall be carried out in search of tumors.1,14
The clinical course of lung evolution is not properly elucidated, and lung function tends to be preserved.3,4 In some cases, there is a decrease in the diffusing capacity for carbon monoxide, particularly when there are multiple, big cysts; thus, when important changes occur in them, we suggest taking lung function tests. Up to now, there isn’t any well-known specific treatment, and no suitable response has been observed with mTor inhibitors. 3,4
As part of the complementary management, we recommend starting with the tobacco cessation program and administering the pneumococcal and influenza vaccines. 3,4,7,9,10,13-15 A pneumothorax management program shall be provided, inclu ding recommendations and warning signs. We recommend that pleurodesis is performed after the first pneumothorax episode, given its high frequency and recurrence; and, in cases of recent pneumothorax, we suggest to the patient that he/ she shouldn’t take non-pressurized flights or prac tice diving, since that may accelerate or worsen the pneumothorax.3,4,7,9,10,13-15
CONCLUSION
The Birt-Hogg-Dubé syndrome is a rare disease that requires high clinical suspicion in order to begin its diagnostic approach. It should be sus pected in patients with skin and renal neoplasia and lung cysts, particularly in cases with familial history of these conditions. The study of this syn drome is part of the differential diagnosis of cystic lung disease and corresponds to the third cause of that disease, which in comparison with other etiologies, doesn’t have many symptoms from the respiratory point of view, with little alteration of the pulmonary function. In turn, it is essential to carry out the screening of first-degree relatives and follow-up of reported lesions. The approach requires multidisciplinary management together with dermatologists, urologists, nephrologists, geneticists and pulmonologists.