Chronic obstructive pulmonary disease (COPD) is an important public health problem because there is growing evidence of the increase in diffe rent epidemiological parameters of considerable concern.1 Smoking is the main cause of COPD.2,3 The smoking prevalence has been decreasing from rates of around 40%, at the beginning of this century, up to near 22% of the general population, according to the national Health Survey of our cou ntry.4 The age of smoking initiation in our country is 14 years; the age of regular consumption is 18, and a tendency to increase consumption is obser ved, particularly in the areas of young people of low income.2,4 Clearly, smoking cessation is still the main therapeutic intervention that improves mor bidity and mortality. 2,3 It is important to highlight the underdiagnosis reflected in several European studies, of around 75% of the total number of patients with COPD.5-7 In the PLATINO study of five cities of Latin America, 82% of COPD patients were unaware that they had this disease, with 77.4% in the Argentinian prevalence study, EPOC.AR.8,9 COPD prevalence in the urban general po pulation of Argentina is 14.3%, but in a sample of a population of more than 40 years with exposure to tobacco (PUMA study) it is higher (29.6%), thus estimating between 2.5 and 3 million patients with COPD.10 With regard to mortality, according to the WHO, it is still the third cause of death, and 80% occurs in countries of low- or middle- income.11 Preliminary studies about COPD mortality in our country show 112% growth compared to 1980, and reaching almost 27 deaths per 100,000 inhabitants in 1998, approximately 5000 deceased, especia lly women.12 Recently, the National Institute of Respiratory Diseases “Dr. Emilio Coni” reported approximately 30,000 annual hospitalizations in part of the public sector in 2015.13
With respect to the morbidity, COPD is the fifth cause of hospitalization in Argentina in individuals older than 60 years.3 In the United States of North America, hospitalizations have increased between 1978 and 1994 from 259,000 to 500,000 per year, especially in individuals older than 65 years.15 As a disabling disease, COPD will go up from the current 12th place to the 5th place throughout the world.16 The increasing cost of chronic diseases has required the analysis of the impact of the diseases on the health system, the cost structure, and the approaches that tend to optimize the system, since the demand is always growing and not satisfied, and health-related costs increase year after year. The progressive increase in life expectancy, the use of diagnostic techniques that are becoming more and more costly, and more expensive treatments had to be weighted in relation to the savings generated by the reduction in the use of health resources, the increase in survival and the improvement in different health markers, such as quality of life.16-22 The National Heart, Lung, and Blood Institute (NHLBI) of the United States acknowledged USD 23.9 billion in COPD expenses, 61.5% for direct costs. The cost per person was USD 1,522 per person, per year, three times higher than the cost of asthma and 2.5 times higher than not-COPD.15,21 The highest costs were the direct costs for hospitalization and visits to the emergency department (72.8%).22 In a study on emphysema costs in Great Britain, from the National Institute for Health of the United Kingdom, Guest et al determined an expenditure of £19 million (approximately USD 34 million) to treat 134,000 emphysema exacerbations (direct costs): 50% for hospitalization costs to treat 3% of total exacerbations.23 The average hospitalization cost was USD 3,600 versus USD 128 for exacer bations treated on an outpatient basis. For that reason, strategies have been created to reduce the number of hospitalizations and their length.23,24 The average hospital stay was 9.9 d. The mean estimation per hospitalization was £ 3,000 (USD 5,700) as opposed to £ 100 (USD 190) for outpatient treatment.24 There are other multiple U.S and European publications about the cost structure of COPD, all of them with the common denominator of the high percentage of hospitalization due to exacerbation and oxygen therapy, which severely impacts on the total cost of this disease.25-44
In Argentina, there is only one publication from twenty years ago about the impact on directs costs of hospitalizations for exacerbated COPD: 33 patients in 1999, in a public hospital of the Gover nment of the City of Buenos Aires.36 The cost per discharge was USD 2,451, with an average stay of 15 d, at USD 163 per hospitalization day.36
The purpose of this study was to describe the direct cost per each hospitalization for COPD exa cerbation and to determine the cost structure in a public hospital of the city of Buenos Aires in 2018.
MATERIALS AND METHODS
We reviewed the medical records of patients hospi talized for exacerbated COPD in every area of the Hospital General de Agudos Dr. J. M. Ramos Mejía of the Autonomous City of Buenos Aires (CABA) from January 1st, 2018 until December 31sr, 2018. Adults older than 18 years were included. Patients with COPD (GOLD definition: FEV1/FVC ratio < 0.70 and postbronchodilator predicted FEV1 < 80%2), older than 40 years, with smoking history (more than 20 packs of cigarettes per year). Pa tients with history of other respiratory diseases were excluded.
Direct costs were determined from the funder’s perspective, taking into account the cost of medi cations and the modulation of the Government of the City of Buenos Aires (GCBA, for its acronym in Spanish) for hospitalization in the intensive care unit (ICU) and regular ward in June 2021. The values of the government’s modulation for public hospitals by June 2021 were: ARS 14,143 (USD 139) for hospitalization in the ward, per patient, per day; non-critical emergency room, ARS 2,957 (USD 30); emergency room including tests, ARS 5,231 (USD 51.5); critical emergency room, ARS 33,070 (USD 325); at the ICU, without mechanical respiratory assistance (MRA), ARS 29,527 (USD 290); and with MRA, ARS 33,070 (USD 325) per patient, per day.45 Each module had certain pre-established number and type of service (biochemistry, imaging, electrocardiogram, spiro metry, MRA, oxygen, disposable material, drugs, etc., apart from the rate that depends on salaries, taxes and charges, administrative fees, equipment amortization, food and laundry costs, etc.). Whe never a patient had any additional consultation, diagnostic practice or treatment (for example, drugs) outside modulated fees, the cost was cal culated from the funder’s perspective according to the KAIROS pharmaceutical vademecum and the list of services of the GCBA nomenclature.46 Given the varying peso/dollar parity, results shall be reported in dollars. The exchange rate used to calculate the cost in dollars was based on the quote of the Banco Nación on June 30th, 2021 ($ 101.17 = USD 1).
The eosinophilia value was obtained before the administration of systemic corticosteroids at the laboratory of the emergency department.
The spirometry was performed the last hospita lization day, before discharging the patient.
Descriptive statistics were used. For quanti tative variables with non-Gaussian distribution, we used the median as central measure and the interquartile range 25%-75% (IQR 25%-75%) as dispersion measure. In order to have a gaussian distribution, we used the mean as central measure and standard deviation as dispersion measure, and for qualitative variables, we used percentages.
RESULTS
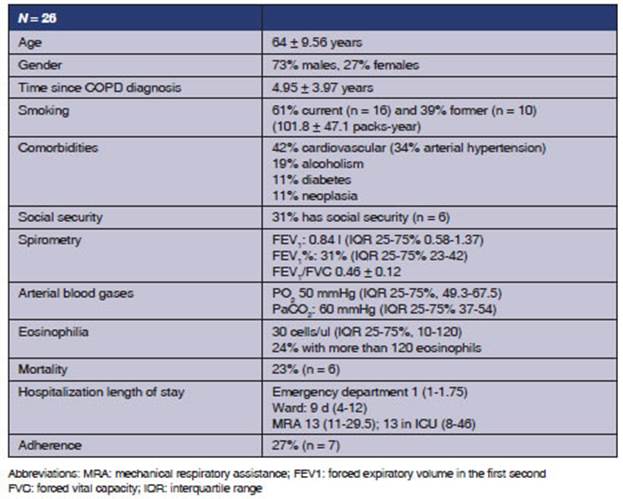
During 2018, 26 patients were hospitalized: 23 in the regular ward and 3 in the ICU. Table 1 shows the demographic characteristics.
Most patients (n = 18 patients [70%]) belonged to the programmatic area of the hospital. From all the patients, only 38.6% (n = 10) had been treated in our hospital before their consultation. Adherence to treatment before hospitalization was poor (27%).
Upon admission, 50% (n = 13) of the patients were receiving treatment with short-action beta- 2 adrenergic bronchodilators; 23% (n = 6), with combination of short-action beta-2 adrenergic and anticholinergic bronchodilators; 15% (n = 4), with a combination of long-action beta-2 adrenergic bron chodilators and inhaled corticosteroids; and 11% (n = 3), with long-action anticholinergic bronchodilators. None of the patients were treated with triple therapy.
Three of the 26 patients (11.5%) were hospita lized twice.
Direct cost analysis
The final direct cost per hospitalized patient in the regular ward was USD 1,462.62 (IQR 25%- 75%, 763.85-2,915.95), which considering the 26 hospitalized patients, gives a total direct cost of USD 117,480, that is, USD 162.44 per patient, per day.
The final direct cost per hospitalized patient at the ICU was USD 9,898.28 (IQR 25%-75%, 6,700.94-35,780.25). Taking into account the fact that only three patients were hospitalized at the ICU, there was an important dispersion of the total direct cost per patient. The total amount spent for three patients was USD 75,064.11.
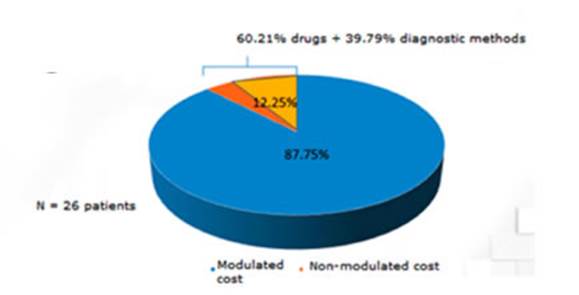
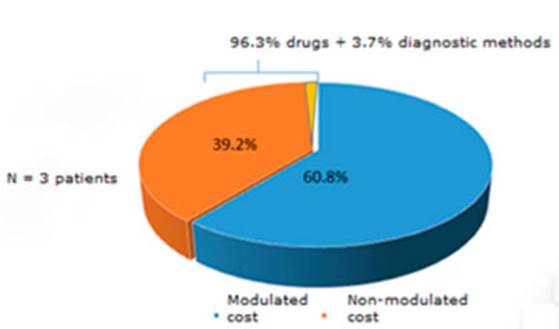
With regard to the direct cost structure, 87.75% of it had been considered inside the clinical module of the GCBA. However, 60.21% of the rest (12.25%) was related to drugs not included in the module, and 39.8% to diagnostic practices not included in the module (Figure 1). But, if we consider ICU hospitalization, 39.2% of the direct cost wasn’t modulated (three times higher than patients hos pitalized in the regular ward). The cost of drugs (specially antibiotics) was the main cause of non-modulated direct cost (96.3%) (Figure 2).
DISCUSSION
The direct cost of exacerbated COPD hospitaliza tion in a public hospital in the Autonomous City of Buenos Aires has been established. The sample consisted of 26 patients, mostly males aged in their 70s, with recently diagnosed disease, high smoking load and severe obstruction of the airflow. The cost in the regular ward was USD 1,462 per patient, and almost seven times higher in the ICU. Patients hospitalized in the regular ward were included in the expected cost module, whereas those from the ICU had a higher percentage outside the module, due to the use of high-cost drugs. The pharma cological treatment profile of most patients in public hospitals in CABA is not included in the recommendations of current guidelines, since it is mainly based on the use short-acting broncho dilators, surely due to the difficulty with access to medication and poor adherence to follow-up.
For the European Union, total annual direct costs of respiratory diseases account for 6% of the total healthcare budget; COPD represents 56% (38.6 billion Euros).2,47 In United States, total annual direct costs for COPD are calculated in USD 29.5 billion, and indirect costs, USD 20.4 billion.2, 48 The highest proportion is related to COPD exacerbation care, which determines a di rect relationship with the severity of the disease. Probably in underdeveloped countries the indirect cost is higher than the negative impact on the direct cost.2,36-43
Given the fact that mortality only offers a limited perspective of the impact of a disease on the human being, Murray et al designed a DALY indicator (Disability-Adjusted Life Year) that was analyzed in the Global Burden of Disease Study; it is the sum of years of life lost due to premature death adjusted by the severity of the disease and concomitant impairment of quality of life.49 So, in 2005 COPD was the eighth cause of DALY lost in the world, and it was estimated that in 2013 it was the fifth cause worldwide, though second in the United States, after coronary disease.49
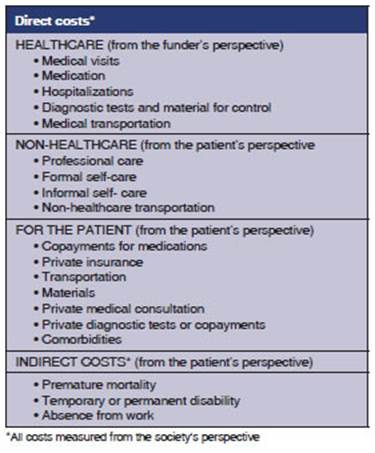
The Asthma Management Spanish Guidelines (GEMA, for its acronym in Spanish) have deter mined the different elements of the direct and indirect cost of asthma, which can be extrapolated to another chronic obstructive disease, such as COPD. The Guidelines recommend forty seven features to be used in a cost study (Table 2).50 Our study implements those recommendations. A mixed methodology has been used to determi ne direct costs: modulation of costs provided by the GCBA (top-down method) and, apart from reviewing all medical records, covering patient’s consumption outside the modulation (bottom-up method). In our study, direct primary data have been collected from the medical records, and that is very valuable information.50 As we have already mentioned, we conducted the cost study from the funder’s perspective (GCBA) in the environment of a public general acute care hospital, thus, the conclusion will only be extrapolated to that health system. Cost comparison between countries or di rect extrapolation are not recommended, because cost structure and health systems vary from one country to another, although it may help by giving us an idea of the magnitude of the problem and the qualitative strength of each variable.50
Bilde et al published a study on Medicare spen ding per person, comparing COPD patients with non-COPD patients. They determined that the cost was USD 8,482 versus USD 3,511 (2.5 times higher). 50% of the cost of COPD is consumed in 10% of the patients.51 Other authors have reported the economic impact of COPD on the North Ameri can Health System. The average days/bed was 7.75 d, but with higher rates of rehospitalization and higher expenses. The average cost was USD 6,469 per patient (direct costs), 68% of which belonged to hospitalizations.48,52 It has already been said that the National Heart, Lung, and Blood Insti tute (NHLBI) of the United States acknowledged a COPD cost of USD 23.9 billion: 14.7 billion were direct costs (61.5%) and 9.2 were indirect costs (38.5%). The cost per person was USD 1,522 per year, three times higher than the cost of asthma and 2.5 higher than non-COPD patients.15,21 The hospitalization index was 21.2 patients for every 1000 persons. The highest direct costs were from hospitalization and visits to the emergency department (72.8%). The rest was divided: 15% for outpatient visits and 12.2% for cost of drugs. But the distribution of COPD expenses was very disproportionate: 10% of patients used 73% of the total expenses.15,21 The increase in the number of hospitalizations was observed in patients older than 45 years. The NHLBI report includes a com parison within respiratory diseases, between the distribution of direct and indirect costs of COPD with asthma, influenza, pneumonia, tuberculosis and lung cancer.15 COPD uses twice the amount of asthma, and compared to influenza, lung cancer or pneumonia, it shows a higher proportion of direct costs.15 Guest et al, in the first study on emphy sema costs in Great Britain, from the National Institute of Health of the United Kingdom, deter mined a cost of £ 19 million (approximately USD 34 million) to treat 134,000 exacerbations due to emphysema (direct costs): 50% for hospital costs to treat 3% of total exacerbations.23 The average cost per hospitalization was USD 3,600 versus USD 128 in exacerbations treated on an outpatient basis. This allowed the creation of strategies to reduce the number of hospitalizations and their length.17 Again, Guest et al conducted another study, similar to the previous one, but taking into account the general COPD costs in the National System of Health of the United Kingdom. An amount of £ 817.5 million (USD 1.553 billion, approximately) was determined, only including direct costs.24 This is equivalent to £ 1,154 per person per year, around USD 2,300 per person per year.24 The average stay was 9.9 days. Hospital expenses were 35% of the total to treat less than 2% of exacerbations.24 The mean calculation per hospitalization was £ 3,000 (USD 5,700), as opposed to £ 100 (USD 190) for outpatient treatment.24 Probably this analysis underestimates the real cost for the society, since it doesn’t consider indirect costs (loss of produc tivity, because COPD has 6 times more absence from work than asthma), direct costs for the pa tient (trips), or intangible costs (quality of life). If we analyze the distribution of direct costs in the United Kingdom, 47.5% was used for the purchase of drugs; 24.5% for home oxygen therapy; 17.8% for hospital fees and 10.2% for medical outpatient fees.23,24
With regard to COPD hospitalization in Argen tina, the National Institute of Respiratory Disea ses “Dr. Emilio Coni” has informed that in 2015 almost 30,500 hospitalizations were reported for exacerbated COPD in a sample including public institutions of the country.13 In the GCBA, in 2013, there were 1,066 hospitalizations, and in 2014, 996 hospitalizations for exacerbated COPD.53
According to the previous cost analysis in pa tients with exacerbated COPD, twenty years ago, including 33 patients, the total direct cost per hospitalized patient was USD 2,451. The structure of hospital costs was distributed as follows: costs of final services represented 75% of total costs; 57% of those belonged to salaries (17.55% for physicians, 37.41% for nurses and 1.51% for administrative employees), and 13% to drugs, disposable ma terials and medical practice (drugs; 8.8% of the total amount).36 The remaining 25% was related to the transfer of costs from general services and other services, with 12.48% for the staff.36 The hospitalization day was USD 163, the same as the cost per hospitalization day of the current analy sis (USD 162), that is to say, it remained stable throughout two decades. It is worth mentioning that oxygen therapy provided at the emergency department, the regular ward and ICU represents a high hospital cost in all the cost analyses of the disease. In our case, it is considered as part of the hospitalization module, just like the use of invasive and non-invasive ventilation is considered within the ICU module. At the time this study was being conducted, the high-flow oxygen cannula wasn’t available.
Regarding the mean hospitalization days of our current study, it has been reduced to 9 days, which is a lot less than the average of this same institution twenty years ago (15 days). The average number of hospitalization days is similar to the one reported internationally: 9.9 d in Great Britain and 7.75 d in the United States.22-24,36 One possible explanation could be that the standardization of treatment and permanent training of healthcare staff in our institution for the adequate and upda ted management of patients with COPD, as well as the availability of more effective pharmacological treatments, have allowed a significant reduction in hospital length of stay. Different international Guidelines (GOLD, ALAT, GESEPOC and others), plus the Guidelines from the Ministry of Health of our country summarize the recommendations for the effective management of COPD, with broncho dilator therapy as the cornerstone. 2,3,54,55
Both the international and the national Gui delines identify a group of patients who share the fact of having been hospitalized the year before or more than one outpatient exacerbation requiring antibiotics or systemic corticosteroids (GROUPS C and D of the GOLD Guidelines). Given the worst prognosis of patients who have suffered frequent exacerbations, with higher impairment of the pulmonary function, symptoms, quality of life and mortality, the frequent exacerbator phenotype is considered by all the Guidelines as the risk factor with the worst prognosis, and deserves a more intensive treatment, even with the use of inhaled corticosteroids. 2,3,54-57 Other factors known as hospitalization risks in COPD are: difficulty in accessing the pharmacological treatment, nonad herence, inhalation errors and comorbidities. 2,3,54,55 In our study, only 10% of patients had social se curity. Also, the high prevalence of mistakes in the administration of inhaled drugs in patients with chronic obstructive diseases, such as asthma and COPD, is well-known around the world.58 Usmani et al determined that advanced age, low socioeco nomic status and low educational level, the lack of previous training in the correct inhalation therapy, and the presence of comorbidities were the factors associated with the mistakes in the administra tion technique; all of this related to bad asthma control and an increase in the use of healthcare resources.59 With respect to comorbidities, there was high prevalence in our study (Table 1), and it is known that they have a bearing on the worst disease prognosis, both in the exacerbator phenotype (groups C and D) and in the non-exacerbator group (Group B).2,3,54,55,60,61
Regarding the limitations of this study, we can say that data collection from the medical records was retrospective. Another limitation is the fact that the extrapolation of conclusions for other health systems in our country or other regions (external validity) is not recommended, due to the different cost structures, as we have already mentioned. Indirect costs haven’t been evaluated (they are thought to be higher than direct costs, basing on previously reviewed information), and costs haven’t been determined from other pers pectives (patient or society). Costs were initially calculated in pesos, but due to the exchange rate instability and the devaluation suffered by our country in the last years we decided to express the results in dollars. Finally, the modulation used by the GCBA didn’t allow us to separate the internal cost structure to know which variables have been considered, and to what extent.
To conclude, after twenty years, a direct cost study of COPD exacerbation in hospitalized pa tients in a public hospital of CABA has been carried out again. The sample consists mostly of men older than 60 years, with poor follow-up, high smoking load and severe obstruction of the airflow. The direct cost from the funder’s perspective was USD 1,462 per patient; the cost of a patient hospitalized at the ICU was almost seven times higher. But we have to take into account that only three patients were admitted to the ICU, and there was great dispersion in the cost per patient. Most of the costs for ward hospitalizations had been calculated in the module, but not in the case of the ICU, which uses high-cost drugs. A significant reduction has been shown in hospitalization length of stay, but with a day-bed cost that remained stable throughout 20 years (USD 162-163). Probably the indirect cost is much higher. We suggest the need to include this type of study in the hospital environment for the purpose of collecting data to allow a better management of the available resources. Including cost-related problems in every affected area could contribute to the management of available resou rces, the planning, organization and systematiza tion of patient care, thus improving the production and quality of the end-product with equal or lower budget. Being the management of COPD patients the most important element of direct costs, syste matic COPD management programs shall be im plemented for the purpose of identifying patients with risk factors, educating them about treatment adherence and allowing access to medication, in order to reduce the number of hospitalizations for exacerbations and, why not, the mortality.