Introduction
Chronic Obstructive Pulmonary Disease (COPD) is a respiratory condition characterized by airflow limitation1,2. It affects more than 5% of the population and is associated with high morbidity and mortality3,4.
According to the WHO (World Health Organization) estimates, 65 million people suffer from mild to severe chronic obstructive pulmonary disease (COPD). The assessments show that by 2030, COPD will be the world’s third leading cause of death5.
In the 2015 review of Dal Negro et al it was observed that patients with COPD showed cardiovascular, metabolic, digestive and osteoarticular comorbidities6.
The GOLD guidelines (Global Initiative for Chronic Obstructive Lung Disease) of 2011, establish that comorbidities affect the “severity” and prognosis of the disease and introduce CHAPTER 6: “As sociated Comorbidities”7.
The 2013 chronic obstructive bronchopathy (COBP) cohort of Burgel et al shows the impact of co morbidities on the quality of life of COPD patients8.
COPD has been associated with several comorbidities that significantly affect the morbidity and mortality of these patients9.
The most common cause of death in patients with severe or very severe COPD is respiratory failure. But in mild-to-moderate COPD patients, mortality is associated with cardiovascular comorbidities and lung cancer10.
The first scientific communication regarding comorbidities of a cohort of COPD patients was shown at the 2015 Congress of the Argentinian Association of Respiratory Medicine (AAMR, for its acronym in Spanish) with the following name: “COPD Comorbidities at the Central Region of the Country” and established the mortality risk through the COTE Index11.
There are well-known indices that evaluate the comorbidities of different chronic diseases12-17.
The Charlson Index, published in 1987, assesses comorbidities associated with chronic diseases with the purpose of evaluating the risk of death in hospitalized patients in a more objective manner12,13.
The COTE index is based on 10 diseases and has been developed for patients with COPD17.
The objective of this study is to compare the Charlston and COTE indices and relate them to mor tality in a cohort of COPD patients followed during ten years.
Materials and Methods
Prospective, observational, cross-sectional cohort study, December 2016. The study included patients with COPD (GOLD 2017 definition) classified according to their severity: GOLD 1 with post-bron chodilator FEV1 > 80% of the predicted value in relation to FEV1/FVC < 0.7; GOLD 2 with FEV1 between 79-50%; GOLD 3 with FEV1 between 30-49% and GOLD 4 with FEV1 ≤ 29%; also taking into account the modified combined assessment of COPD in ABCD groups exclusively based on symptoms and history of exacerbations18.
Also, functional evaluations were carried out ( spirometry and 6-minute walk test). We calculated the BODE index (body-mass, airflow obstruction, dyspnea, and exercise) and assessed comorbidities through the BODE, Charlson and COTE indices, with survival follow-up from 1996 to December 201612,13,17,19. We evaluated mortality according to the vital status from the date of diagnosis to December 31, 2016.
The Charlson index has 19 medical conditions classified in four groups according to the importance assigned to each disease. In 1994, Charlson et al validated the combined use of comorbidity and age12,13.
The COTE index, created with 10 diseases, showed a mortality predictive value that is independent from the BODE index; and a score of ≥ 4 increases the predicted risk of death in every quartile of the BODE more than twice17.
Statistical analysis
Continuous variables were expressed in mean ± standard deviation (SD, in case of Gaussian distri bution) or median and interquartile range 25 and 75 (CI 25-75, in case of non-Gaussian distribution). Categorical variables were expressed in percentages. For the correlation test we used the Pearson’s linear test. An alpha error of p< 0.05 was considered significant.
Results
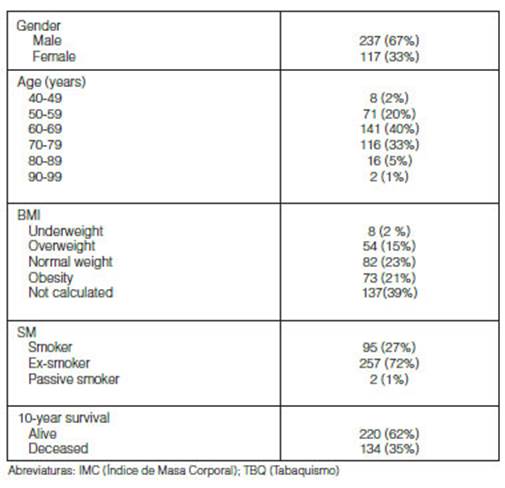
Table 1 shows the demographic characteristics.
We included 354 COPD patients: age 66.5 ± 8.4, 66.7% male, 74.2% ex-smokers, (56 ± 29.7 p/y). After ten years, 220 patients were alive (62%) and 134 had died (38%), follow-up 28 (12-54.7) months (median, CI 25-75%) (Table 1).
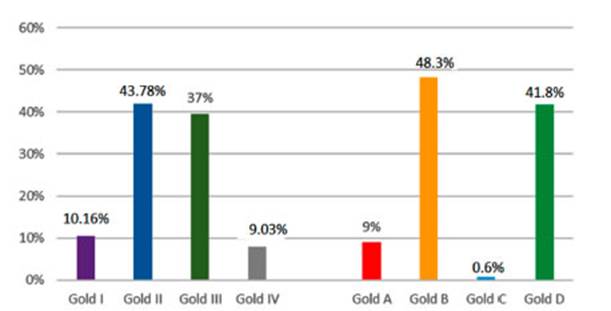
They had the following classification: GOLD 1 (10.16%), 2 (43.78%), 3 (37%), 4 (9.03%); A (9%), B (48.3%), C (0.6%) and D (41.8%) with a mean post-bronchodilator FEV1 of 53.8 ± 20% (Figure 1).
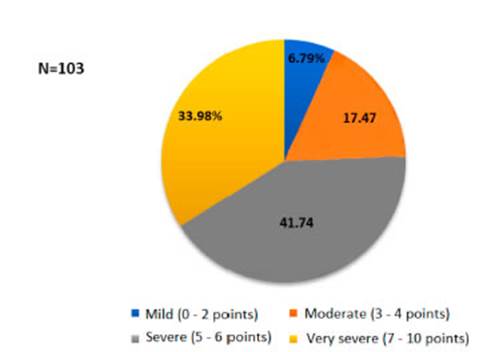
The average distance covered in the 6-minute walk test was 294.76 ± 160.8 meters and the BODE score was: mild (6.79%), moderate (17.47%), severe (41.74), and very severe (33.98%) with an average of 5.5 ± 1.9 points (Figure 2).
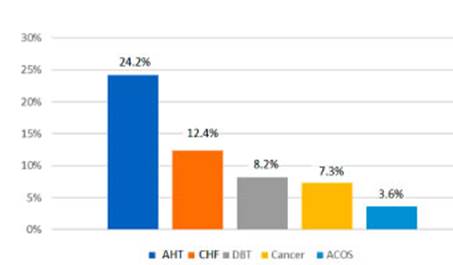
The most common comorbidities were: arterial hypertension (AHT) 24.2%, congestive heart failure (CHF) 12.4%, diabetes (DBT) 8.2%, cancer 7.3% and asthma-COPD overlap syndrome (ACOS) 3.6% (Figure 3).
The diseases with higher mortality rates were CHF 21%, AHT 11.2%, DBT and cancer 8,2%, AMI 6%, OSAHS and ACOS 1.5%, and AF 0.75%.
Also, most comorbidities occurred in patients with Gold stages B and D and those with mild and severe degrees of obstruction.
AHT, CHF, AMI, and DBT were the most common comorbidities.
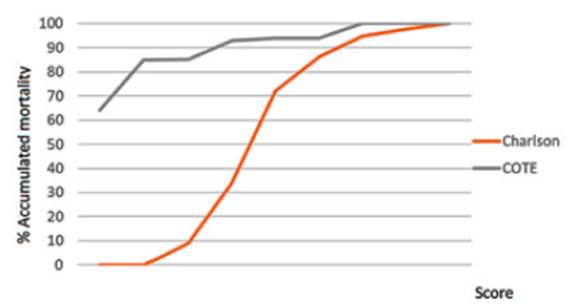
The mean Charlson index was 4.1 ± 1.7. A cut-off point of ≥ 4 discriminates 66% of deceased patients. The mean Charlson index was 0.8 ± 0.1. 85% of deceased patients have one point or less in the COTE index (Figure 4).
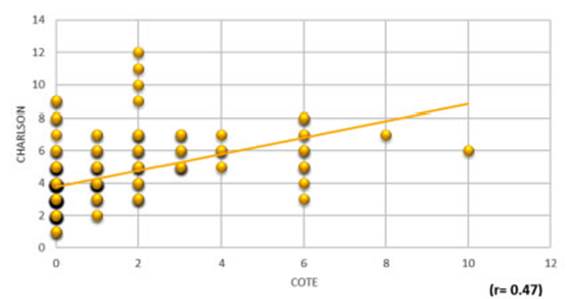
The COTE index correlates poorly with the Charlson index (r = 0.47) (Figure 5).
Discussion
In a cohort of more than 350 patients with COPD who were followed up for twenty years in a Department of Respiratory Medicine, most comorbidities were shown in patients of GOLD stages B and D, with moderate and severe degrees of obstruction; and AHT, CHF, AMI and DBT were the most common comorbidities. There was a poor correlation between the Charlson and COTE indices. A Charlson index score of ≥ 4 more accurately discriminated mortality compared to the COTE index.
Cardiovascular diseases and diabetes are the most prevalent comorbidities in patients with COPD, and the ones mostly related to mortality.
In the different cohorts such as ECLIPSE and PLATINO, the presence of comorbidities in COPD is of great relevance and determines mortality in this kind of patients20,21. The most frequent comorbidities in the ECLIPSE study were osteoporosis, anxiety and cardiopathies. The presence of cardiopathies and diabetes mellitus increased the probability of death and even a C cluster was established, called inflam matory COPD with comorbidities, where it was observed that this group showed a worse survival rate during follow-up20. In the PLATINO study, most frequently reported diseases in the 5 cities were arterial hypertension and cardiovascular diseases; the latter were associated with higher rates of mortality21.
Most of these comorbidities were found in patients with moderate and severe degree of obstruction and groups B and D.
Ana López et al showed in 2015, from a total of 811 evaluated patients: an elevated prevalence of comorbidities (mean of 3.55 diseases x patient), morbidity > 90% of the sample with > 2 comorbidities; the cardiovascular disease was the most common comorbidity, psychiatric diseases were in third place as regards frequency, with more anxiety than depression, a high prevalence of comorbidities in early stages of COPD, higher percentage of comorbidities in stages B and D, low COTE index for the general sample (2.25) and higher risk of mortality in more symptomatic groups (B and D)12.
The Charlson index was proposed by Mary Charlson et al in 1987 with the purpose of developing a prognostic instrument of comorbidities that could have an impact on the short-term mortality risk of patients included in research studies, either individually or in combination. It was initially adapted for the evaluation of one-year survival, but finally adopted its definite form to analyze survival after 10 years12.
In 1994, Charlson et al validated the combined use of comorbidity and age14. A score of 1 is assigned to myocardial infarction, congestive heart failure, peripheral vascular disease, cerebrovascular disease, dementia, COPD, connective tissue disease, ulcerous disease, mild liver disease and diabetes. A score of 2 is assigned to diabetes with terminally damaged organ, hemiplegia, renal disease and malignant neoplasm, including leukemia and lymphoma. A score of 3 is assigned to moderate or severe liver disease, whereas AIDS (acquired immunodeficiency syndrome) and metastatic malignant tumors are assigned a score of 6. Results showed that the relative risk of death for every decade of age was 1.42 (95% CI = 1.08- 1.88), and for every increment in the degree of comorbidity, it was 1.46 (95% CI = 1.22-1.74). So, the estimated relative risk adjusted for every unit (age/comorbidity) was 1.45 (95% CI = 1.25-1.68)11,12.
The Charlson Index, published in 1987, assesses comorbidities associated with chronic diseases with the purpose of evaluating the risk of death in hospitalized patients in a more objective manner, allowing us to know the prognosis of patients with comorbidities in the geriatric population12,13.
The COTE index is based on 10 diseases and has been developed for patients with COPD17. The values are obtained by adding up the scores assigned to the patient’s diseases: if the result is ≥ 4, it is associated with a 2 or 3-fold increase in the risk of death17.
A poor correlation has been shown between the two most widely used indices to evaluate comorbi dities (Figure 5). The Charlson index of ≥ 4 points more accurately discriminates mortality (66% of deceased patients), which is not the case with the COTE index (85% of deceased patients have a 0 to 1 score) (Figure 4). We believe this has to do with the fact that the COTE index doesn’t adequately score the diseases that establish an important rate of mortality in patients with COPD.
Divo et al designed a prognostic influence study, in terms of mortality, of comorbidities associated with COPD. A total of 79 comorbidities were reviewed and even though AHT, dyslipidemia and obs tructive sleep apnea were the most prevalent, they didn’t have a significant mortality risk. Only 12 of the diseases that were found were independently associated with risk of death in patients with COPD: lung cancer, anxiety in the female population, pulmonary fibrosis, hepatic cirrhosis, atrial fibrillation, diabetic neuropathy, heart failure and ischemic cardiopathy. The authors believe this index is easier to calculate than the Charlson index, and better predicts the risk of mortality17.
Almagro et al evaluated the impact on mortality after hospitalization for COPD. It was observed that patients with 3-point Charlson index (corresponding to 2 chronic diseases or one disease other than COPD) had twice the possibilities of dying, as post-hospitalization predictor of mortality (P > 0.0006), regardless of age, gender or FEV1. The most frequently associated comorbidity was chronic heart failure, and it was the only significant comorbidity in the bivariate analysis (p 0.001: OR 2.3; CI 1.39 to 2.83)13.
In 2010, in a new study by Almagro et al including 398 patients with COPD, the most common co morbidities were arterial hypertension (55%), arrhythmias (27%) and diabetes mellitus (26%). 27% had heart failure, 17% coronary disease and 9% had previous myocardial infarction with a Charlson index score of 2.72. No relationship was found between hospital mortality and the number of comorbidities (p = 0.8) or the Charlson index (p = 0.6)14.
The PROFUND study from Spain reported a mean Charlson index score of 3.99, which is clearly higher than that described by Almagro et al in 2010. Cardiovascular diseases, diabetes, dyslipidemia, renal failure and anemia have been the most common comorbidities. It has been observed that, the higher the number of comorbidities, measured with the Charlson index, the higher the mortality rate15.
To conclude, in a cohort of patients with moderate to severe COPD, with predominance of group B and D who were followed for twenty years, the most commonly found comorbidities were AHT, CHF, AMI and DBT. A poor correlation has been shown between the two most widely used indices to evaluate comorbidities. A Charlson index score of ≥ 4 points more accurately discriminates mortality, in compa rison with the COTE index. It is important to identify comorbidities in a COPD patient because they are related to a worse quality of life, and an increase in the use of healthcare resources and mortality.