INTRODUCTION
State-of-the-art science promotes constant experimentation with different materials that are biocompatible with the human body, because innovation in dental biomaterials is essential to improving the practice of medicine and regenerative dentistry 1-3 . Dental biomaterials are those materials used in regenerative 4 , prosthetic and reconstructive dentistry with the goal of replacing missing tissue as closely as possible to the original. To be considered acceptable, a biomaterial must be biocompatible, have good adhesion, have natural appearance similar to that of the missing tissue, be bioinert, bacteriostatic, bactericidal, and importantly, not cause toxic damage to the cells surrounding the tissue to be treated 5 , 6 . Chitosan is a biopolymer with bactericidal/bacteriostatic effects, biodegradable and biocompatible 7 , which has been used in tissue engineering to replace tissues partially or completely by releasing bioactive materials or influencing cell growth 7 , 8 .
Tissue regeneration is the answer for comprehensive restitution of body tissue after injury, unlike repair, where the scar tissue is formed with different features from the original tissue 9 . Every year, over 500,000 grafting procedures are performed to restore functionality following injuries such as bone fractures, injuries resulting from a variety of surgical, degenerative disease and traumatic causes that can be disabling or even cause loss of stability 9 , 10 . Bone and other tissue grafts have been an essential tool for rehabilitation in oral mucosa and other body parts because of their inductive capacity to regenerate damaged tissue caused by trauma or surgical treatment. Tissue engineering creates artificial grafts that are able to induce newformation and regeneration of soft and hard tissues through natural regeneration processes 11 .
Hemostatic gelatin is a product obtained during the degradation of collagen triple helical structure into single molecules. For years, gelatin has received much attention as a hemostatic material due to its excellent properties such as low antigenicity, biocompatibility, biodegradability and relatively low cost. Gelatins are also widely used in the sustained release of drugs and tissue engineering applications with bone, cartilage and skin 12 , 13 . It has been reported that gelatin can activate platelet aggregation and it is also used as an absorbable hemostatic agent 14 . The mixture of gelatin and polymers increases its chemical stability, improves mechanical properties and bioactive properties such as biocompatibility and antimicrobial effects. Chitosan has good filming and viscosity, contains free amino groups and can cross-link with gelatin 15 . These characteristics of gelatin and chitosan enable them to form a natural semi-interpenetrating polymer network among molecules and acquire porous properties similar to biological scaffolds 15 , 16 . However, few studies have been performed on the combination of chitosan and gelatin 17 .
Although some studies have been conducted on the cell cytotoxicity of chitosan 7 , 18 , the current study includes three different types of cell cultures. The objective of this research was to determine the cytotoxic and anti-inflammatory effects of chitosan alone or with an impregnated hemostatic gelatin scaffold (Spongostand®) in culture on human gingival fibroblasts (HGF), human pulp cells (HPC) and mouse pre-osteoblasts (MC3T3-E1), through a series of experiments of dose-response curve and expression of prostaglandin E2 (PGE2) with MTT and ELISA assays 19 , 20 . All assays were conducted at the Interdisciplinary Research Laboratory; Nanostructures and Biomaterials Area of the National School of Higher Studies, Unit León UNAM.
MATERIAL AND METHODS
Cell culture
The protocol was reviewed by the institution’s bioethics committee for the patients’ cell isolates and accepted under number CE_16/004_SN. All patients gave their permission for their extracted teeth to be used in this research.
To obtain human pulp cells (HPC) and human gingival fibroblast (HGF), non-pathologically damaged erupted third molars and gingival tissue were collected from healthy patients who underwent surgical odontectomy of third molars. After extraction, the samples were stored in Falcon® tubes with 10 mL of phosphate buffer saline (PBS, pH 7.4) and 1% antibiotic (Gibco®, Grand Island, NY, EU). Each molar was cut at the cementoenamel junction with a carbide disc using a low-speed turbine under constant irrigation. The pulp and gingival tissue were obtained inside a laminar flow chamber (Lumistell®, Celaya Gto., Mexico) and explants of about 1x1 mm were performed with scalpel blade #20 in 60x15mm culture dishes (Thermo Fisher Scientific, Rochester, NY, EUA). The explants were inoculated into sterile 100x15mm culture dishes (Thermo Fisher Scientific) with DMEM culture medium supplemented with 20% Fetal Bovine Serum (FBS, Gibco®), 1% antibiotic (10,000 UI/ mL penicillin G and 10,000 μM/mL streptomycin sulfate, Gibco®), and 1% Glutamax (Gibco®). They were incubated at 37 ºC with 5% CO2 and 95% humidity (Binder, Tuttlingen, Germany) for 3 weeks until a cellular confluence monolayer of 80% was obtained. The culture medium was replaced every third day after the first week. Mouse pre-osteoblast cells (MC3T3-E1, mouse C57BL/6 calvaria) were obtained from a certified strain (ATCC® CRL-2593) and sub-cultured in DMEM culture medium added with 10% FBS, 1% antibiotic and 1% Glutamax. Cells were sub-cultured in a range of 2x105 cells/mL for each experiment.
Chitosan and gelatin preparation
Chitosan was prepared from shrimp shells 0.1gr/10mL (<75% deacetylation, Sigma Aldrich, Toluca, Mexico), mixed and stirred with 1% acetic acid. The mixture was left stirring on the heating and stirring grill at room temperature for 24 hours until it was homogenized and viscous-looking. The chitosan was prepared at 0.19% and the hemostatic gelatin (Spongostan®, Ethicon, Johnson-Johnson, Belgium) was impregnated.
Cell Viability
HPC, HGF and MC3T3-E1 were sub-cultured in DMEM medium at 2x105 cells/mL in 96-well dishes and incubated for 48 h at 37ºC with 5% CO2 and 95% humidity. Chitosan was inoculated at different concentrations in a range of 0-0.5% and incubated for 24 hrs. In case of hemostatic gelatin impregnated with 0.19% chitosan, the cells (HPC and HGF) were inoculated in a 24-well plate and the scaffolds were placed in direct contact for 24 hours. A control group of scaffolds was mixed with saline solution. Finally, the culture medium was removed and replaced by MTT reagent (0.2 mg/mL, thiazolyl Blue Tetrazolium Bromide, 98% Sigma Aldrich), incubated for 7 hours, and the crystals of formazan were dissolved with dimethyl sulfoxide [(CH3)2SO, DMSO, J.T Baker, USA]. The plate was analyzed in a microplate spectrophotometer (Thermo Scientific Multiskan GO) at 570 nm wavelength. The cells of the 24-well plate were transferred to 96-well plates to analyze mitochondrial metabolic activity. Each test was performed in triplicate for each of the three independent experiments.
Anti-inflammatory activity
HGF was sub-cultured as described above in 24- well plates. Interleukin-1β (recombinant human IL-1β, >97% Purity, R&D Systems, Minneapolis, MN, USA) reconstituted with albumin (Bovine Albumin Solution, 22%, IMMUCOR GAMMA, Norcross, GA, USA) was used to induce cells to a pro-inflammatory state (3 ng/mL) and use them as a positive control for 3 h 19 , 20 . Then, the hemostatic gelatin scaffolds impregnated with chitosan at 0.19%, 1% and saline solution were inoculated in 24-well plates and incubated for a further 24 hours. The culture medium supernatant was stored in Eppendorf tubes, and prostaglandin E2 (PGE2) expression was analyzed with an expression kit (R&D Systems) with ELISA tests, following the manufacturer’s instructions.
Statistical analysis and data expression
Means, standard deviations and percentages were calculated. The data were analyzed with Shapiro- Wilks normality test, paired Student t-test to compare incubation times of cell proliferation, and ANOVA post hoc Tukey test. Significance was set at 0.05 and reliability coefficient 95%.
RESULTS
All the data were adjusted to normal distribution. Fig. 1 summarizes the dose-response curve of the cytotoxic activity of chitosan from 0 to 0.5%. The viable cell number was reduced significantly. The results from most to least sensitive to contact with chitosan were HPC(CC50=0.11±0.04%) <HGF(CC50=0.19±0.02%) <MC3T3-E1(CC50=0.19±0.03%).
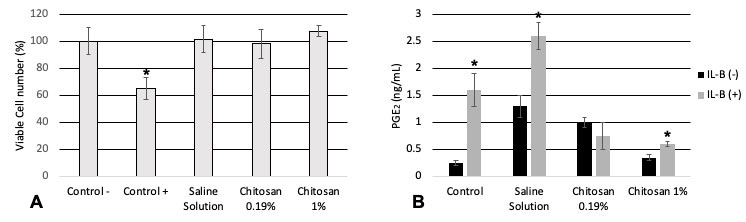
Fig. 1 Cytotoxic activity of chitosan in culture with HGF, HPC, MC3T3-E1 for 24 hours of incubation. The relative viable cell number was determined by the 3-[4,5-dimethylthiazol- 2yl]-2,5-diphenyltetrazolium bromide assay. Each value represents the mean±S.D. of triplicate assays, *p<0.05 paired Student-t test (Intragroup), ANOVA Tukey test (Intergroup), n=9.
The direct contact of hemostatic gelatin scaffolds impregnated with chitosan at 0.19% showed a cell viability as follows: HPC: Control (Saline solution)= 94.98±1.55%, Chitosan 0.19%=89.14±0.57%; HGF: Control (Saline solution)=61.43±2.98%, Chitosan 0.19%=11.90±0.04%. The contact with HGF significantly reduced the viable cell number (p<0.05, Student-t test, n=9).
The individual cell viability tests were conducted using MTT on the HGF with hemostatic scaffolds (Fig. 2A) impregnated with chitosan or physiological solution for the control group, with and without IL-1β. An increase in cell viability of 106.91% was observed in chitosan with IL-1β. Then, a test was performed with prostaglandin E2 and ELISA analysis. The following results were observed with the tests used to measure the pro-inflammatory effects using Prostaglandin E2 (PGE2): the cells that were inflammed with IL-1β expressed a greater amount of PGE2 alone and with physiological solution, while in contact with Chitosan 0.19% and 1%, PGE2 expression was reduced significantly (p<0.05) (Fig. 2B).

Fig. 2 Anti-inflammatory effect of hemostatic gelatin (Spongostand®) impregnated with chitosan by the synergistic stimulation of PGE2 production with IL-1β. A) Near confluent HGF cells were pre-treated to induce inflammation for 3 h with IL-1β (3 ng/mL) and incubated for a further 24 hours. The relative viable cell number was determined by the 3-[4,5-dimethylthiazol-2yl]-2,5-diphenyltetrazolium bromide assay. B) The concentration of PGE2 in the culture medium was determined by ELISA, to induce cells to a pro-inflammatory state (3 ng/mL) and use it as a positive control for three hours. Each value represents the mean±S.D. by triplicate assays. *p<0.05, **p<0.01 paired t-test, n=9.
DISCUSSION
Other studies prior to ours have shown that chitosan has healing and antimicrobial effects. A systemic study conducted in Madrid on its cytotoxicity established that the lethal dose in rats (LD50) was 16g/kg. The healing and bactericidal effect of chitosan has also been proven in studies conducted in Peru and Mexico 2 , 6 , 21 .
There is a need for new regeneration techniques for the oral mucosa –different from the tissue grafts used currently– which would be suitable for use in humans and applicable in restorative dentistry and oral surgery. The natural biopolymer chitosan satisfies these needs. Mexico is one of the countries with the most coasts and production of crustaceans from which chitosan can be obtained 2 , opening a broad panorama in terms of producing chitosan for regeneration techniques.
Our research team at the ENES Leon of the UNAM set itself the task of testing, standardizing and investigating the cytotoxic effects of chitosan in contact with human gingival fibroblasts (HGF), human pulp cells (HPC) and mouse osteoblasts (MC3T3.E1). HGF and HPC are common in the oral cavity. When they were placed in contact with chitosan –both in solution and in hemostatic sponges– in vitro, mean cytotoxicity concentration (CC50) was found to be 0.19%. It has been shown that Schwann cells and endothelial cells enhance attachment, proliferation, and survival rates 22 .
With regard to anti-inflammatory effect, it has been shown that chondrocytes cultured in chitosan alginate beads reduce the expression of inflammatory cytokines (IL-6 and IL-8) and increase cartilage matrix component (hyaluronan and aggrecan) synthesis in vitro, in comparison to alginate beads alone 23 . Moreover, chitosan scaffolds have been found to inhibit the release of IL-1β and thus the formation of inflammasomes in mouse and human macrophages in vitro 24 . Here, we reported the potential anti-inflammatory effect by reducing the PGE2 released form human gingival fibroblast previously induced to gingivitis.
As mentioned in our hypotheses, at chitosan concentrations greater than 0.19% in contact with human pulp cells (HPC), human gingival fibroblasts (HGF) and mouse osteoblasts (MC3T3-E1), chitosan produces cytotoxic effects; however, at concentrations<0.19%, cell viability is higher in these cell lines, where at the same time their natural biopolymer characteristics continue to be maintained, as well as their recently known antiinflammatory effect. The current research studied properties of chitosan related to uses in medicine, and now dentistry. In the future, formulations could be based on the knowledge gained. Chitosan as a single biomaterial or in combination with other polymers could provide great improvements in tissue engineering and regenerative medicine, by providing a safe, affordable alternative for any type of condition, and helping to improve healing in situations such as oral surgery, periodontics, implantology, or any other requiring optimal, safe grafts. In the future, more studies will focus on the preparation of chitosan scaffolds via 3D printing and cryogelation methods to facilitate the application of chitosan in biomedicine. Chitosan, as a part of any material, could introduce valuable properties such as antimicrobial activity, mucoadhesion, and biocompatibility, which are required properties for a regenerative biomaterial.
Our results indicate that chitosan at concentrations above 0.19% can induce cell death or decrease cell viability when in direct contact with human pulp cells (HPC), human gingival fibroblasts (HGF) and MC3T3-E2. However, at concentrations lower than or equal to 0.19%, it induces cell viability and does not cause cytotoxicity, at the same time having a significant anti-inflammatory effect. Considering both the findings and the limitations, a new potential application of chitosan using a hemostatic gelatin scaffold for formulations in regenerative dentistry is proposed.














