INTRODUCTION
Cancellous bone architecture provides appropriate information about the biomechanical characteristics of bone 1 . For decades, conventional histomorphometry has been the gold standard for analyzing trabecular bone microarchitecture. However, it only enables two-dimensional measurements (2D) of specific, small sections of bone, and is invasive, time consuming, and predisposes to sampling errors. In recent years, micro-computed tomography (pCT) devices have been validated and are now the gold standard for quantifying bone microstructure 2 . The pCT technique enables detailed assessment of 3D trabecular bone microstructure. However, because it causes high radiation exposure, it can be only used in vitro for small samples. Cone-beam computed tomography (CBCT) has spatial resolution similarto that ofconventional pCT but, particularly for trabecular bone, has relatively low cost and requires a lower dose or effective radiation 3 . In recent years, CBCT has emerged as a feasible, non-invasive, accurate tool for the assessment of several parameters of trabecular bone microarchitecture, including bone volume fraction (BV/TV%), trabecular thickness (TbTh) and trabecular spacing (TbSp) 4 . These parameters are important to evaluating trabecular bone quality, and the CBCT technique enables their quantitative examination 5 .
Postmenopausal osteoporosis is a metabolic disorder characterized by low bone mass and microarchitectural deterioration of bone tissue, which increases the risk of bone fractures. The primary clinical diagnostic criteria for osteoporosis are based on the decrease in bone mineral density (BMD) 6 . Nonetheless, bone architecture, too, affects the risk of bone fractures. Bisphosphonates (BPs), which are synthetic analogues of pyrophosphate, have traditionally been used to treat postmenopausal osteoporosis and other metabolic bone diseases 7 . BPs are rapidly cleared from systemic circulation and located on bone mineral surfaces, particularly at sites of high osteoclast activity, because of their high affinity for the calcium of the hydroxyapatite crystal 8 . Nitrogen-containing BPs inhibit the mevalonate pathway in the osteoclasts, decreasing cell activity and the rate at which bone is remodeled. Although they prevent loss of bone mass, their effect on bone quality is still not clear.
Bone remodeling enables bone tissue to adapt to different physiological conditions, and to replace damaged bone with newly formed bone. Even though trabecular bone remodeling is similar throughout the skeleton, jawbone remodeling is faster and constant because of the mechanical loading stimulus (forces) during mastication, particularly in alveolar bone 9, 10 , 11 . The high reduction in bone turnover, especially with the most potent BPs, such as zolendronic acid (Zol), could affect the microarchitecture and biomechanical properties of bone. In this regard, BP-related osteonecrosis of the jaw (BRONJ) has been characterized as one of the main side effects of chronic therapy with BPs 1 2 . Sheep have long been used in bone research because they are large, docile animals that are easy to house and handle, and have low maintenance costs 13 . They are comparable to humans due to their weight, size and bone similarity, and have often been subject to research in maxillofacial areas 14, 15 , 16 . They have molars and premolars with periodontium similar to humans, experience age-related skeletal problems including tooth loss, and develop periodontitis with similar oral pathogenic bacteria to those found in the human oral environment 17 . Ovariectomized (OVX) ewes showed a remarkable decrease in BMD 18 . As in humans, the OVX ewes treated with high doses of BPs for a long time could develop BRONJ 16 .
In dentistry, CBCT is still limited to evaluating bone density in the jaw 19 , 20 . However there is a strong demand in clinical practice for quantitative analyses of bone microstructure. We hypothesize that CBCT has high potential for the diagnosis and treatment of osteoporosis. It is thus important to determine whether it is sensitive enough to identify changes in jawbone microstructure after bone loss or specific treatments. The aim of this preliminary report was to use CBCT analysis for assessing quantitative trabecular changes in the lower jawbone associated with high bone loss and antiresorptive treatment.
MATERIALS AND METHOD
Animals
Twelve virgin adult Corriedale ewes (3-4 years old), with 35 to 40 kg body weight (BW) were used for this study. They were housed, treated, and then euthanized by veterinarians authorized to handle animals by the “National Service for Health and Agro-Food Quality” (SENASA: “Servicio Nacional de Sanidad y Calidad Agroalimentaria”). BW was recorded once a month till the end of the study 16 .
All procedures were performed in compliance with
Buenos Aires University’s Hospital de Clínicas “José de San Martín” ethics guidelines approved on December 26, 2016. The animals were housed at the experimental farm of Río Negro National University and fed a daily ration of standard dry sheep feed with hay, wheatgrass, and grasses to meet nutritional recommendations. Water was supplied ad libitum.
Drug administration
In humans, intravenous amino-BPs injections are used to decrease bone resorption in several bone pathologies (e.g., osteoporosis, bone metastases, multiple myeloma, hypercalcemia of malignancy). To ensure high accumulation of BP in bone in order to induce a drastic decrease in bone resorption, the ewes were administered the most potent amino-BP at higher doses. The drug administration schedule and dose were in keeping with a published regimen for treating myeloma patients 21 . Fasting ewes were administered 4 mg Zol/month (equivalent to 66 pg/ kg for 60 kg of BW) by jugular injection for 28 months. In order to rule out confounding factors and evaluate exclusively the effect of BP accumulation on the jaw, no other drug known to suppress the immune system (e.g., glucocorticoids) or inhibit it (e.g., bevacizumab) was administered.
Experimental design
The experimental design was previously published by our group 16 . Briefly, a veterinarian surgeon performed bilateral OVX on 8 animals and sham surgery (SHAM) on 4 animals under general anesthesia and cardiac and respiratory monitoring, following standard protocols for this type of procedure 22 . Two days post-surgery, OVX ewes were divided into two subsets and treated for 28 months (T=28) as follows:
OVX: OVX ewes receiving 10 mL of saline solution by jugular injection.
OVX+ZOL: OVX ewes treated with 10 mL of a Zol solution (4 mg/month) to obtain a high cumulative dose of Zol in the bone.
SHAM: SHAM ewes receiving 10 mL saline solution and serving as controls
At T=28 animals were euthanized, and hemi-mandibles were excised and cleaned of soft tissue. Immediately after excision, they were analyzed by densitometry and computed tomography. Then, the hemi-mandibles were washed with saline and immersed in ethanol 60 % (v/v) for 72 hours. The alcohol was replaced at 24 hours intervals. The samples were dried in an oven at 100 °C for 24 hours and weighed.
Densitometry
Hemi-mandible BMD and bone mineral content (BMC) were evaluated ex vivo by dual energy x-ray absorptiometry (DXA) (Lunar DPX) using a software specifically designed for animals. All bones were scanned using an identical scanning procedure. Hemi-mandibles were analyzed on a bone image on the screen. Software precision for mandible BMD was assessed by measuring one piece of mandible five times after repositioning between scans both on the same and on different days 15 . The hemi-mandible coefficients of variation (CVs) were as follows: BMD=0.8 % and BMC=3.0 %. All analyses were performed by a single blinded technician, to minimize inter-observer variation.
Imaging Studies
The hemi-mandibles were analyzed by computed tomography at 1:1 magnification (Tomograph Gendex CB-500, Cone Beam, Georgia, USA). The digitalized images were analyzed using a 2D Image Analysis Software (Image Pro Plus 4.5, Media Cybernetics, USA) at the Department of Oral and Maxillofacial Radiology at Río Negro National University.
CBCT images were taken at 200 mm field of view, 120 kV, 300 minutes, scanning time 0.5 second/ rotation, and slice thickness 0.5 mm with a high-resolution model. The CBCT analysis was performed using Planmeca Promax 3D Classic. Field of view was set at 80x80 mm, and voxel size at 200 pm3. Each maxilla was scanned with tube current 9 mA, voltage 105 kv, and exposure time 9 seconds. The trabecular bone histomorphometry parameters measured by CBCT were analyzed using Image J2 23 with BoneJ2 plug-in 24 . CBCT scans were imported into the software. Images were calibrated in mm and default threshold was applied. Five cuboids were obtained from each hemi-mandible, including only cancellous bone, endeavoring to cover the entire tomography trabecular bone. TbTh, TbSp, BV/TV%, connectivity density (CD) and degree of anisotropy (AD) were calculated.
Statistical analysis
IBM SPSS Statistics for Windows Version 21.0 (IBM Corp. USA) was used. A value of p<0.05 was considered significant. Data were expressed as mean ± standard deviation (SD). Normality of variables was evaluated using the Shapiro Wilk test, and homogeneity of variances was assessed by Levene’s test. Data were analyzed using one-way analysis of variance (ANOVA) to detect differences in percentages and means, followed by multiple comparisons using Bonferroni’s post hoc test.
RESULTS
No significant difference in BW was observed among groups, either at the beginning or at T=28 (Table 1). At the end of the study, the significantly lowest hemi-mandible weight was observed in OVX (p<0.05), and the significantly highest value in OVX+ZOL (p<0.05) (Table 1).
Hemi-mandible BMC and BMD values were significantly lower in OVX than in SHAM and OVX+ZOL (p<0.01); no statistical difference was observed between OVX+ZOL and SHAM (Table 1). CBCT analysis showed that BV/TV% (Fig. 1), TbTh, CD and AD were significantly lower (p<0.0075; p<0.0075, p<0.001 and p<0.02, respectively), and TbSp was significantly higher (p<0.0002) in OVX than in SHAM (Fig. 2A-D). AD was significantly higher (p<0.018) and TbSp significantly lower in OVX+ZOL than in OVX (p<0.043) (Figs. 2D and 2B, respectively). BV/TV%, TbTh and CD showed a clear tendency to be higher in OVX+ZOL than in OVX (p=0.055; p=0.061 and p=0.054, respectively) (Figs. 1, 2A, and 2C). No statistical difference in the CBCT parameters was observed between OVX+ZOL and SHAM.
Table 1 Body and maxilla weight, bone mineral content and density at the end of the study Body and maxilla weight, bone mineral content and density at the end of 28 months of treatment. Data were analyzed by one-way ANOVA followed by multiple comparisons using Bonferroni’s post hoc test. Results were expressed as mean ± SD. Different letters indícate statistically significant difference. BW: body weight; BMC: bone mineral content; BMD: bone mineral density.
| Experimental Groups | BW (Kg) | Maxilla weight (g) | BMC (g) | BMD (g/cm2) |
|---|---|---|---|---|
| SHAM | 29.7±2.8 | 178.4±4.0 b | 37.2±2.9 b | 0.244±0.016 b |
| OVX | 30.7±4.6 | 142.8±2.3 c | 24.0±6.1 a | 0.166±0.040 a |
| ZOL | 32.0±2.8 | 185.1±5.7 a | 42.3±3.0 b | 0.254±0.026 b |
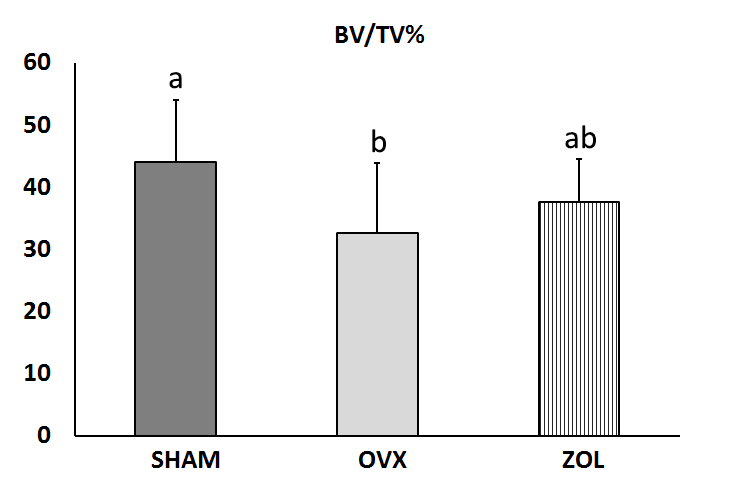
Fig. 1 Change in the jawbone volume (BV/TV%) measured by CBCT in the three experimental groups. Data were analyzed by one-way ANOVA followed by multiple comparisons using Bon-ferroni ’s post hoc test. Results expressed as mean ± SD. Different letters indicate statistically significant difference (p<0.05).
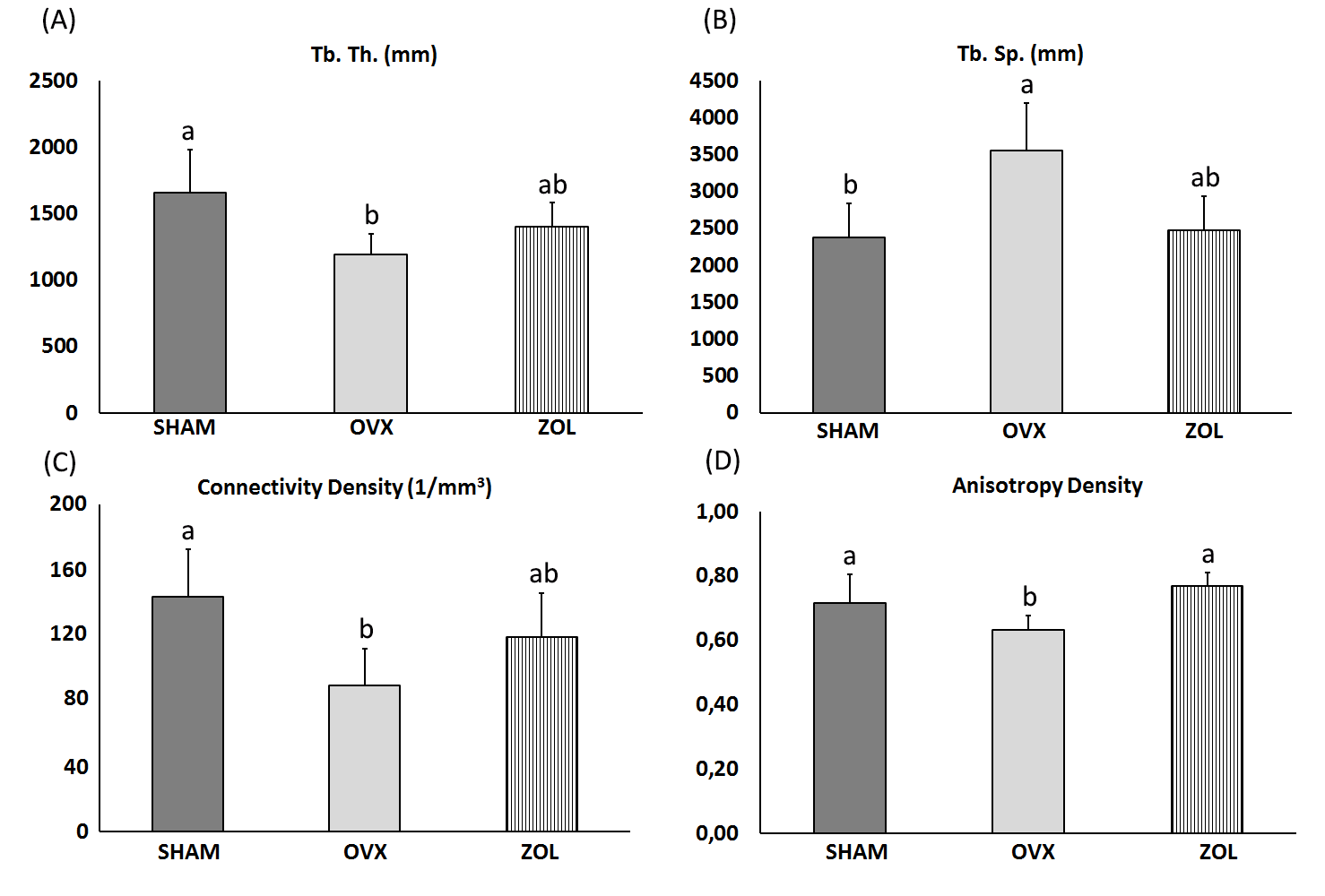
Fig. 2 A) Bar graphs of trabecular thickness (TbTh), B) trabecular spacing (TbSp), C) connectivity density, and D) anisotropy density, measured by CBCT in the three experimental groups. Data were analyzed by one-way ANOVA followed by multiple comparisons using Bonferroni’s post hoc test. Results expressed as mean ± SD. Different letters indicate statistically significant difference (p<0.05).
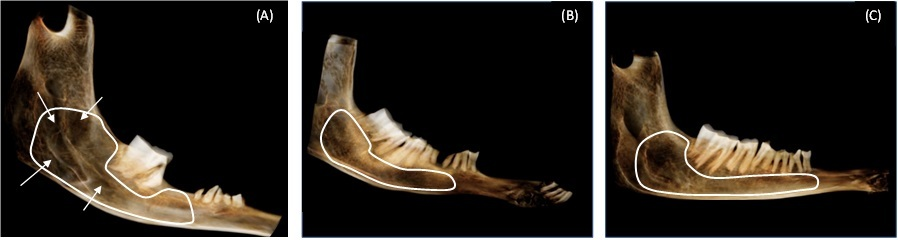
Fig. 3 Panoramic tomography of the lower left jaw of SHAM (A), OVX (B) and ZOL (C) groups. The zone delimited in white corresponds to the area of analysis by the CBCT technique. Arrows show the reduced radiodensity area in the OVX group as compared to SHAM and ZOL groups. The latter two show similar levels of radiopacity
The area of analysis of CBCT is shown in Fig. 3. The tomography of the hemi-mandible shows normal radiodensity in SHAM and OVX+ZOL (Fig. 3A and 3C). The arrows point to the areas of low radiodensity in OVX (Fig. 3B).
DISCUSSION
The present preliminary report evaluated the usefulness of CBCT for assessing the quantitative changes in jawbone microarchitecture after estrogen withdrawal and antiresorptive treatment. The comparative analysis of the results showed that the jawbone quality of the ewes, as occurred in bone density, was seriously affected after 28 months post-OVX, and although the loss of bone density was prevented by the treatment with high doses of Zol, the microstructural parameters were only partially recovered.
Animal models are very important to understanding several aspects of the pathological mechanism of bone diseases, as well as to establishing prevention and management strategies. Most basic investigations in this field have been conducted in rats 25 . Ewes are large animals that provide a suitable experimental model for many reasons. They are closer than rodents to humans in genetic constitution and metabolic rate (0.22 vs. 0.21); they undergo Haversian bone remodeling, and like women, they have menarche and regular, frequent ovulatory cycles. Bone metabolism in the OVX sheep resembles that of women during early postmenopause 26 , 27 .
Estrogen is an important regulator of bone homeostasis. The decline in estradiol levels accelerates bone remodeling characterized by higher bone resorption than bone formation, leading to bone loss over time 28 . The animal model of estrogen withdrawal is ovariectomy. In the present report, as expected, bone mass and density had decreased by 30% at T=28. In addition to bone mass, the composition and microstructure arrangement of the basic components of bone play a critical role in the ability of the jawbone to support mastication. Indeed, the load required for bone deformation is proportional to BMD, and therefore to the degree of bone matrix mineralization. However, the spatial distribution of bone mass (i.e., microarchitecture) influences the biomechanical efficiency of bone to support loads. It has been estimated that bone quantity is responsible for 60 to 80% of the biomechanical resistance of the bone, while the remaining 20-40% depends on bone quality 29 .
The term bone quality comprises a set of bone tissue characteristics encompassing múltiple aspects of bone physiology, degree of mineralization, morphology and type of trabecular pattern which, in addition to density, contribute to bone strength 30 . According to the literature, BV/TV%, TbTh and TbSp are the most crucial indices for determining the trabecular bone microarchitecture 31 . However, it is important to note that trabecular bone is anisotropic, and that the inclusion of structural anisotropy improves the assessment of bone strength. In the present report, the evaluation of lower jawbone quality included these indices. The reference values were obtained by analyzing the lower jaw of the SHAM control group, which characterizes the physiological bone microarchitectural state. Any changes in these values were considered as having been induced by ovariectomy and anticatabolic treatment.
Under the experimental conditions in the current study, the CBCT technique showed that ovariectomy induced a mean loss of 25% in BV/TV%, and decreases of 30% in TbTh, 50% in TbSp, 40% in CD, and only 12% in AD. All these changes suggest an impairment of lower jaw bone mechanical integrity. According to the literature, BV/TV, which is considered one of the most important parameters in bone quality, shows a high correlation with BMD 32 . In this regard, the significant decrease in BV/TV% following ovariectomy observed in the present study may indicate that the trabecular bone strength of the jaw was highly affected. The changes in the bone morphometric parameters detected by CBCT in the lower jawbone of OVX ewes agree with previous findings in other bones, using a different technique. Conventional histomorphometric analysis of the lumbar vertebrae and the iliac crest showed a decrease in BV/TV% and in TbTh, and an increase in TbSp 33 , 34 ; p-CT analysis of femoral neck showed a decrease in BV/TV% and TbTh one year after OVX 35 , 36 , while in the spine or distal femur such changes were observed one or two years after OVX 5 . Connectivity estimates the number of connected structures in a network whose maintenance is critical for supporting loads. CBCT measurement of CD showed a significant decrease in OVX, providing evidence that the trabecular network was seriously altered. This finding is crucial because it has been suggested that for the same decline in bone mass, the loss of trabecular connectivity is 2 to 5 times more deleterious to bone strength than is the thinning of the trabeculae 37 . The high reduction in trabecular separation was not unexpected because in 3-D analysis, this parameter is influenced by connectivity. Anisotropy represents the 3D configuration and arrangement of bone, and it is more independent of bone mass than the other 3D morphometric parameters, so may strongly contribute to predicting changes in bone strength. Our CBCT analysis showed that in OVX, both BV/TV% and the heterogeneity of trabeculae were reduced, suggesting a decrease in the load-carrying capacity and mechanical function of the lower jawbone. All these findings indicate that, as expected, densitometry reveals the loss of bone mass and density by ovariectomy, but CBCT analysis adds information showing that ovariectomy seriously jeopardized the structural resistance of the lower jawbone.
Remodeling enables bone tissue to adapt to different physiological conditions and replace damaged bone with newly-formed bone. Although the bone remodeling mechanism in the jawbone is similar to that in other bones, jawbone is remodeled more rapidly because of the effect of mastication 9 . Excessive osteoclastic bone resorption results in an osteoporotic stage characterized by loss of BMD and biomechanical properties of bone as observed in the OVX ewes. Pharmacological strategies for osteoporosis consist of increasing bone strength and improving bone quantity and quality. BPs are the drugs of choice to initiate anticatabolic therapy for osteoporosis. They are incorporatedfaster in the active areas of osteoclastic bone resorption 6 , reducing the rate of bone remodeling and bone loss. In the current study, treatment with Zol was started immediately after surgery (2 days), preventing the bone loss that occurs as a consequence of the estrogen withdrawal induced by the ovariectomy. In this regard, the results of the present report agree with previous findings showing that preventive treatment with Zol protected against OVX-induced loss of BMD and BMC. However, the CBCT technique showed that bone quality was only partially recovered. Indeed, in OVX+ZOL ewes, BV/TV%, TbTh and CD values were 15% lower than in control ewes, while TbSp and AD values were similar. These results provided evidence that although Zol prevented the decay of cancellous bone mass and density induced by OVX, the recovery of bone microstructure was only partial. It must be taken into account that the main bone quality defect in osteoporosis is the disruption in bone microarchitecture, and that Zol treatment cannot completely restore the mechanical integrity ofjawbone because it lacks an anabolic effect. Traditionally, the evaluation of bone status has depended on bone quantity or bone density; however, if bone architecture is also determined as described in the present report, it is possible to assess bone mass and quality at the same time, enabling a more precise evaluation of bone strength and therefore of the risk of fracture. The results of the present report clearly indicate that high-resolution CBCT is adequate for characterizing and differentiating the microarchitecture of both normal and osteoporotic lower jaws of ewes, before and after antiresorptive treatment. The future standardization of these findings may extend the availability of this technology in basic longitudinal research, laying the groundwork for future use in clinical practice, especially when repetitive follow-up measurements are needed.
Although CBCT technology can be used to evaluate the jawbone in vivo, one limitation of the present study is that the measurements were conducted ex
CONCLUSION
CBCT in a nondestructive, fast, very precise procedure for measuring bone morphometric indices without biopsies, which are not indicated for morphometric evaluation in osteoporosis.
In conclusion, the present study demonstrated the potential of the high-resolution CBCT imaging to evaluate in vivo the quantitative bone morphometry and bone quality of lower jaw cancellous bone in normal condition, and to distinguish the changes associated with excessive bone loss induced by estrogen withdrawal and antiresorptive intervention. Although further studies are needed, these results provide an additional tool for evaluating trabecular mandibular bone microstructure in preclinical studies, laying the groundwork for its future application in clinical practice.















